Home / Health / Breast Cancer: Global Divide Widens
Breast Cancer: Global Divide Widens
3 Mar
Summary
- Breast cancer mortality nearly doubled in low-income countries since 1990.
- High-income nations saw a nearly 30% decline in breast cancer deaths.
- Treatment access and cost are major barriers in poorer regions.
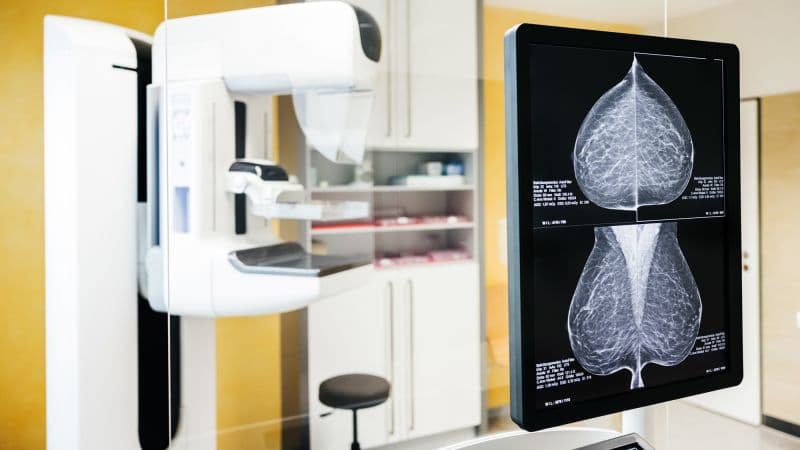
Globally, breast cancer diagnoses are projected to exceed 3.5 million by 2050. In 2023 alone, an estimated 2.3 million women were diagnosed, leading to 764,000 deaths worldwide. While high-income countries have achieved nearly a 30% reduction in mortality since 1990 through improved screening and treatment, the trend is alarmingly reversed in low-income settings.
Over the same period, deaths from breast cancer have nearly doubled in the world's poorest nations, with diagnosis rates soaring by 147%. This widening gap underscores a critical lack of infrastructure for diagnosis and treatment, particularly in regions like sub-Saharan Africa where mortality rates are more than double the global average.
The disparity stems from a mismatch between rising diagnoses and insufficient healthcare infrastructure. Essential treatments like surgery, radiation therapy, and chemotherapy are often unavailable or unaffordable in low-income countries. For instance, a standard course of a targeted therapy can cost as much as a decade's average income in some areas.
Experts emphasize that effective interventions must span the entire cancer care continuum, from early detection to comprehensive management. Political will and investment are crucial to ensure accessible and affordable services, integrating them with broader noncommunicable disease efforts. Without these measures, many countries will miss global targets for reducing mortality.
Even within high-income countries, disparities persist. Black women in the US, for example, face a 40% higher death rate from breast cancer than White women, indicating ongoing challenges in achieving equitable care. Factors such as delayed diagnoses, treatment access gaps, and biases contribute to these internal inequities.
For individuals seeking to mitigate risk, lifestyle adjustments like limiting red meat, quitting tobacco, managing weight, and reducing alcohol consumption are recommended. However, these changes cannot eliminate risk entirely, as many causes are not lifestyle-attributable. Regular screening, such as mammograms every two years starting at age 40 for women in the US, remains a critical tool for early detection.