Home / Health / Psychedelics: Mind vs. Medicine?
Psychedelics: Mind vs. Medicine?
13 Mar
Summary
- Psychedelics are studied for chronic Lyme, Alzheimer's, and PTSD.
- Lyme patient felt significant improvement after psilocybin treatment.
- Scientists debate if drug effects stem from brain chemistry or experience.

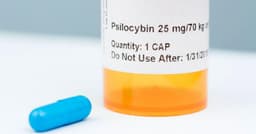
Psychedelics, such as psilocybin from magic mushrooms, are under investigation for treating a wide array of conditions, including chronic Lyme disease, Alzheimer's, and PTSD. Albert Garcia-Romeu, a psychologist at Johns Hopkins University, led a study on psilocybin for post-Lyme disease patients.
One patient, Lori Unruh Snyder, a professor, experienced significant psychological symptoms even after antibiotic treatment for Lyme disease. After participating in the psilocybin study, she reported a transformative shift in her perspective and teaching methods, referring to herself as a 'new Lori.'
Scientists like Boris Heifets, a neuroscientist at Stanford, highlight the challenge of isolating the effects of the drug's impact on brain chemistry versus the transformative personal experiences patients undergo. This difficulty in controlling for subjective journeys complicates research.
Historically, psychedelic research faced a significant halt in the 1970s due to drug crackdowns. The subsequent focus shifted to daily medications like SSRIs, which, while effective for many, leave a portion of patients untreated, creating a demand for alternative therapies like ketamine, and reviving interest in psychedelics.
Determining whether the therapeutic benefits of psychedelics stem from altered brain chemistry or the profound experiential aspects is a central debate. Researchers are exploring ways to untangle these effects to potentially develop treatments that benefit a broader range of individuals, even those who may not undergo a 'trip.'